Frequently Asked Questions

What natural and integrative options are available for managing menopause symptoms in Sydney?
Menopause marks a significant hormonal transition, typically occurring between the ages of 45 and 55, though perimenopause can bring noticeable symptoms for a decade or more beforehand as the body gradually shifts toward the final menstrual period. For some women, this transition is relatively smooth. For others, symptoms such as hot flushes, night sweats, mood... Read more
Read More
How can Ayurvedic lifestyle principles support women’s hormonal health?
Ayurveda is one of the world’s oldest and most comprehensive health systems, originating in India over five thousand years ago. Far more than a collection of herbal remedies, Ayurveda offers a sophisticated framework for understanding how individual constitution, daily routines, seasonal rhythms, food choices, mental patterns, and lifestyle habits interact to create or undermine health.... Read more
Read More
What is nutritional and environmental medicine, and how can it benefit my health?
Nutritional and environmental medicine is an evidence-based medical discipline that examines the profound influence that food, nutrients, and environmental exposures have on health at a cellular and systemic level. It is grounded in the understanding that the body requires specific nutrients to function optimally, and that deficiencies, imbalances, or toxic exposures can disrupt fundamental biological... Read more
Read More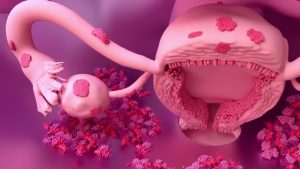
How does functional medicine approach endometriosis differently from conventional treatment?
Endometriosis is a complex, inflammatory condition in which tissue similar to the uterine lining grows outside the uterus, on the ovaries, fallopian tubes, bowel, bladder, and beyond. It affects roughly one in ten women of reproductive age, yet on average takes seven to ten years to diagnose. The impact on quality of life can be... Read more
Read More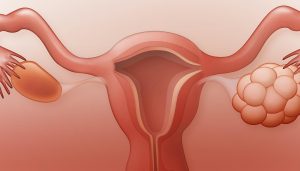
What is PCOS, and how can a functional medicine approach help manage it?
Polycystic ovary syndrome (PCOS) is one of the most common hormonal conditions affecting women of reproductive age in Australia, yet it remains frequently misunderstood, underdiagnosed, and poorly managed in mainstream healthcare. It is not simply a condition of the ovaries. It is a complex hormonal and metabolic syndrome involving irregular or absent ovulation, elevated androgens... Read more
Read More
Can a functional medicine doctor help with unexplained infertility in women?
Unexplained infertility, receiving a diagnosis that tells you nothing is wrong when you have been unable to conceive, can be one of the most emotionally exhausting experiences a woman can face. Standard fertility workups typically assess hormone levels, fallopian tube patency, sperm parameters, and uterine anatomy. When these return normal results, patients are often told... Read more
Read More
How Functional Medicine Finds Chronic Illness Root Causes
Functional medicine approaches chronic illness by looking beyond surface‑level symptoms and examining the deeper patterns that have contributed to your health concerns over time. Chronic conditions often arise from a combination of inflammation, stress, nutrient depletion, gut imbalance, hormonal disruption, and environmental exposures. These influences accumulate gradually, often long before symptoms appear. During your consultation,... Read more
Read More
How Functional Medicine Restores Energy and Vitality
Low energy is one of the most common symptoms in chronic illness, yet it rarely has a single cause. Fatigue often reflects a combination of inflammation, hormonal imbalance, mitochondrial dysfunction, poor sleep, nutrient deficiencies, or chronic stress. Functional medicine evaluates these systems together to understand what is preventing the body from producing and sustaining energy.... Read more
Read More
MindBody Medicine’s Role in Chronic Disease Management
Mind‑body medicine recognises that emotional well-being and physical health are deeply interconnected. Chronic stress, unresolved emotional strain, and nervous system dysregulation can influence inflammation, digestion, immunity, and pain perception. Over time, these factors can contribute to the development or worsening of chronic illness. Mind‑body practices such as mindfulness, breathwork, meditation, or gentle movement help regulate... Read more
Read More
Why Personalised Testing Improves Chronic Disease Care
Chronic symptoms often stem from subtle imbalances that routine tests may not detect. Personalised testing can explore nutrient levels, digestive function, microbiome diversity, inflammation markers, toxin exposure, or hormonal rhythms. These insights help us understand how your body is functioning and where support is needed. This level of detail allows us to create a treatment... Read more
Read More
How Hormonal Imbalances Affect Chronic Health Conditions
Hormones regulate metabolism, mood, sleep, energy, immune function, and reproductive health. When these chemical messengers become disrupted due to stress, poor sleep, nutrient deficiencies, or environmental exposures, the effects can ripple through multiple systems in the body. Functional medicine evaluates hormonal health as part of a broader network. For example, thyroid function may be influenced... Read more
Read More
How Functional Medicine Reduces Chronic Inflammation
Chronic inflammation is a major contributor to many long‑term conditions, including joint pain, digestive issues, fatigue, and metabolic disorders. Unlike short‑term inflammation, which helps the body heal, chronic inflammation persists and gradually disrupts normal biological processes. Functional medicine works to uncover what is keeping the inflammatory response active. This may include hidden food sensitivities, chronic... Read more
Read More
How Integrative Medicine Supports Chronic Disease Care
Integrative medicine combines the strengths of conventional medical care with evidence‑based natural therapies to create a more complete approach to chronic disease. Chronic conditions often involve complex interactions between the immune system, hormones, digestion, and the nervous system. Therefore, a single treatment approach may not be sufficient. Conventional medicine provides essential diagnostics, medications, and acute... Read more
Read More
Lifestyle Medicine for Long‑Term Chronic Disease Support
Lifestyle medicine recognises that everyday habits shape your internal health environment. Over time, the way you eat, move, sleep, and respond to stress can either support healing or contribute to the development of chronic illness. These lifestyle patterns influence inflammation, metabolism, immune function, and energy levels, all essential components of long‑term health. Many chronic conditions... Read more
Read More
How do hormones affect bone health and osteoporosis risk?
Bone is a living tissue that constantly remodels itself. Hormones are key regulators of this process. Estrogen: Protects against bone loss by slowing bone breakdown. After menopause, estrogen levels drop sharply, increasing fracture risk. Testosterone: Supports bone strength in men. A gradual decline with age can weaken skeletal structure. Thyroid hormones: Both excess and deficiency... Read more
Read More
Can hormonal imbalance contribute to mood disorders?
Yes, hormones are closely tied to brain chemistry and emotional regulation. Imbalances can mimic or worsen anxiety and depression. Estrogen: Supports serotonin and dopamine. Low estrogen (e.g. in menopause) can trigger irritability, anxiety, or low mood. Testosterone: Influences motivation, confidence, and resilience. Low levels in men and women can cause apathy, irritability, or mild depression.... Read more
Read More
What role do hormones play in sleep quality?
Hormones are central to circadian rhythm and sleep cycles. When they’re out of balance, sleep often becomes fragmented or restless. Progesterone: Has a calming effect on the brain and promotes deeper sleep. Low levels, common in perimenopause, can cause insomnia and night waking. Cortisol: Should peak in the morning and drop at night. If cortisol... Read more
Read More
How does gut health influence hormone regulation?
Your gut microbiome is deeply connected to hormone balance. It influences how hormones are produced, metabolised, and eliminated. Estrogen balance: The “estrobolome” (a collection of gut bacteria) regulates how estrogen is recycled. If these bacteria are imbalanced, estrogen can build up, leading to heavy periods, PMS, or weight gain. Cortisol and stress: Gut inflammation activates... Read more
Read More
Can chronic stress disrupt hormone balance?
Stress is one of the most underestimated drivers of hormonal imbalance. When your body perceives ongoing stress, whether this be from work, relationships, illness, or even hidden inflammation, it activates the hypothalamic‑pituitary‑adrenal (HPA) axis, releasing cortisol and adrenaline. Over time, this constant “fight‑or‑flight” state disrupts multiple hormone systems. Thyroid function: Elevated cortisol slows the conversion... Read more
Read More
What Role Does Thyroid Function Play in Weight Management?
Your thyroid gland is like your body’s thermostat for metabolism. It produces hormones (T3 and T4) that determine how quickly your body converts food into energy. Underactive thyroid (hypothyroidism): Slows metabolism, leading to weight gain, fluid retention, fatigue, constipation, and cold intolerance. Even mild hypothyroidism can make weight loss frustratingly slow. Overactive thyroid (hyperthyroidism): Speeds... Read more
Read More
Can Improving Metabolic Health Reduce Cardiovascular Risk?
Absolutely in fact, it’s one of the most powerful ways to protect your heart and blood vessels. Poor metabolic health characterised by high blood sugar, high blood pressure, abnormal cholesterol, and excess abdominal fat, increasing the risk of: Heart attack Stroke Peripheral artery disease Heart failure How improving metabolic health helps: Lowering blood sugar reduces... Read more
Read More
What’s the Link Between Insulin Resistance and Hormonal Imbalance?
Insulin resistance occurs when your cells stop responding effectively to insulin, forcing your pancreas to produce more insulin to maintain stable blood sugar levels. Over time, this can lead to chronically high insulin levels, having ripple effects across your hormonal system. In women, high insulin can overstimulate the ovaries to produce androgens (male hormones), contributing... Read more
Read More
How do Hormones Influence Weight Gain or Difficulty Losing Weight?
Hormones act as the body’s metabolic regulators, controlling how you store fat, burn energy, and respond to hunger cues. When they’re in balance, your body can efficiently manage weight. When they’re not, even disciplined diet and exercise routines can feel ineffective. Key players include: Insulin: Moves glucose from the bloodstream into cells for energy or... Read more
Read More
What Lifestyle Changes Support Thyroid and Adrenal Health?
Supporting thyroid and adrenal function requires a holistic approach that balances nutrition, stress management, sleep, and movement. Nutrition Thyroid support: Ensure adequate intake of iodine (seaweed, iodised salt), selenium (Brazil nuts, seafood), zinc (pumpkin seeds, oysters), and iron. Adrenal support: Focus on vitamin C (citrus, capsicum), B vitamins (whole grains, leafy greens), and magnesium (nuts,... Read more
Read More
Is Adrenal Fatigue a Medically Recognised Condition?
In conventional endocrinology, adrenal fatigue is not an officially recognised diagnosis. The adrenal glands are either functioning normally or are in a state of adrenal insufficiency, which is a serious and measurable condition often caused by autoimmune disease or long-term steroid use. However, in functional medicine, adrenal fatigue is used to describe a subclinical state... Read more
Read More
How do Thyroid issues affect Metabolism and Energy levels?
Thyroid hormones act as the body’s metabolic regulators. They influence how quickly cells convert nutrients into energy, how efficiently the body maintains temperature, and how responsive tissues are to other hormones. In hypothyroidism, low levels of T3 and T4 slow down metabolic processes. This can lead to: Fatigue and sluggishness Weight gain and fluid retention... Read more
Read More
What’s the Difference Between Hypothyroidism and Adrenal Fatigue?
Hypothyroidism is a medically recognised endocrine disorder where the thyroid gland produces insufficient thyroid hormones (T3 and T4). These hormones regulate metabolism, energy production, and temperature control. When levels are low, the body slows down, leading to: Persistent fatigue Weight gain despite normal eating habits Constipation and dry skin Sensitivity to cold Depression or slowed... Read more
Read More
What Tests are used to Diagnose Hormonal Imbalance?
Diagnosis begins with a detailed symptom history and physical exam, followed by targeted lab testing. The choice of tests depends on your age, sex, and suspected imbalance. Common blood tests include: Sex hormones: estrogen, progesterone, testosterone, SHBG, LH, FSH Thyroid panel: TSH, free T4, free T3, reverse T3, thyroid antibodies Adrenal function: morning cortisol, DHEA-S... Read more
Read More
How do Menopause and Andropause differ in Symptoms and Treatment?
Menopause and andropause are both age-related hormonal transitions, but they differ in onset, progression, and biological impact. Menopause typically occurs between the ages of 45–55 and marks the end of ovarian function. Estrogen and progesterone levels drop sharply, leading to: Hot flashes and night sweats Vaginal dryness and discomfort during intercourse Mood swings, anxiety, and... Read more
Read More
What are the Signs of Hormonal Imbalance in Women vs Men?
Hormonal imbalances can affect nearly every system in the body. While some symptoms overlap, others are gender-specific due to differences in reproductive hormones. In women, common signs include: Irregular or absent menstrual cycles Premenstrual mood swings, bloating, or breast tenderness Fatigue, low energy, and difficulty concentrating Weight gain (especially around the hips or abdomen) Hair... Read more
Read More
